Pelvic pain and varicose veins are both common conditions that affect many women. While they may seem like separate issues, recent studies have shown a strong connection between the two. Varicose veins in the pelvis, also known as pelvic congestion syndrome (PCS), can cause pelvic pain. At the same time, pelvic pain can lead to poor circulation in the legs, increasing the risk of developing varicose veins. Understanding this connection between pelvic pain and varicose veins is crucial for women’s health and well-being. In this blog, we will explore the causes, symptoms, and treatment options for both conditions.
What are varicose veins?
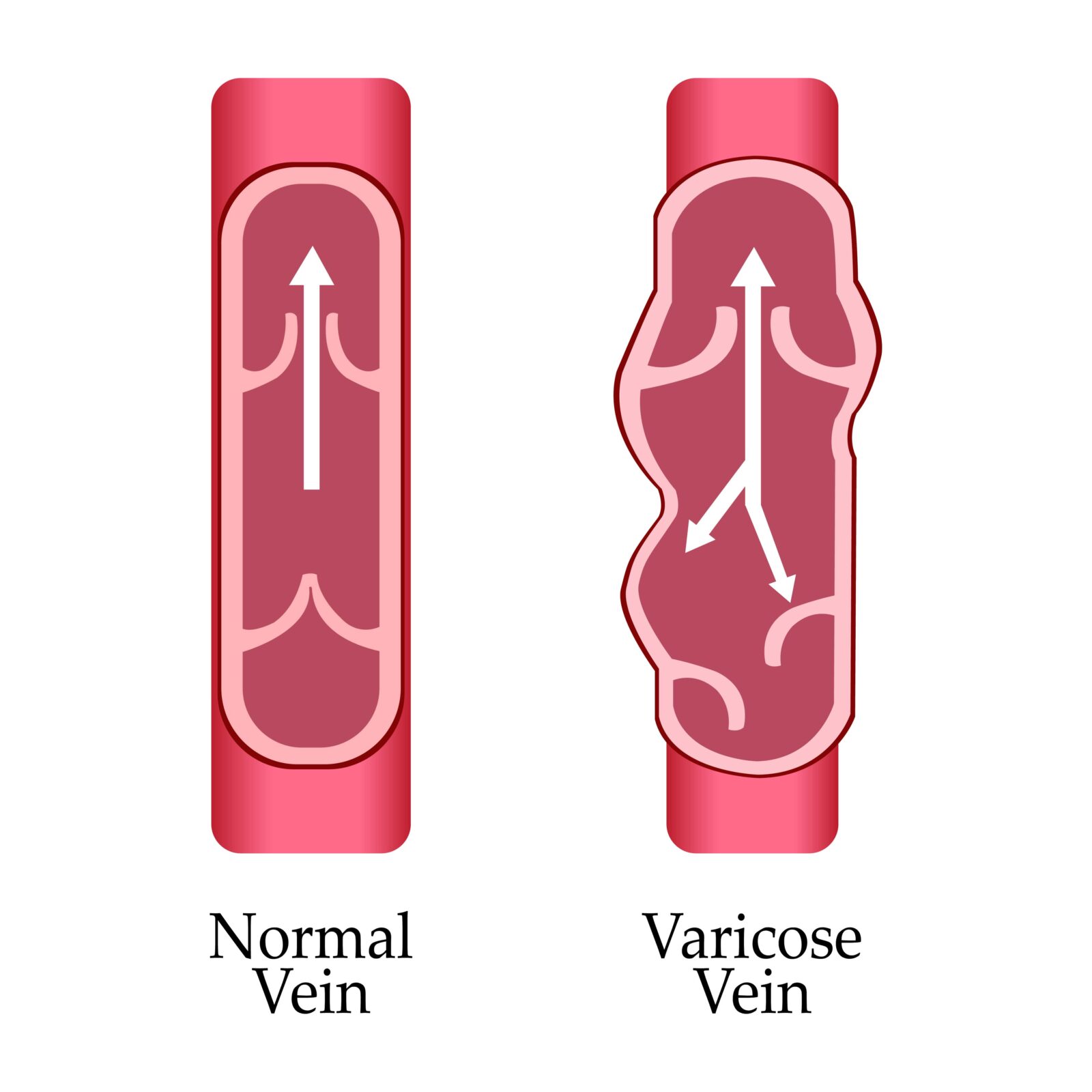
Varicose veins are swollen and enlarged veins that are visible through the skin. They occur when the valves in the veins that prevent blood from flowing backward fail to function properly, leading to the accumulation of blood in the veins. This causes the veins to bulge and become twisted or rope-like in appearance.
Varicose veins most commonly occur in the legs, but they can also develop in other parts of the body, such as the pelvis or anus. They are often blue or purple in color and may cause pain, itching, swelling, and aching in the affected area. Varicose veins can be a cosmetic concern, but they can also cause discomfort and, in severe cases, lead to complications such as blood clots and ulcers.
The causes of varicose veins include genetics, pregnancy, hormonal changes, obesity, and a sedentary lifestyle. Symptoms of varicose veins include pain, itching, swelling, and aching legs.
Understanding Pelvic Pain
Pelvic pain is discomfort that occurs in the lower abdominal area, between the belly button and the groin. It can be caused by a wide range of factors, including menstrual cramps, endometriosis, uterine fibroids, ovarian cysts, and pelvic inflammatory disease.
Risk factors for pelvic pain include age, hormonal changes, pregnancy, and a history of sexual abuse or trauma. Symptoms of pelvic pain can range from mild to severe and may be accompanied by other symptoms such as nausea, fever, and painful urination.
The Connection Between Varicose Veins and Pelvic Pain
Varicose veins in the pelvis, also known as pelvic congestion syndrome (PCS), can cause pelvic pain in women. PCS occurs when the veins in the pelvis become enlarged and swollen, leading to discomfort and pain. The exact cause of PCS is not fully understood, but it is believed to be related to hormonal changes, pregnancy, and genetics. The symptoms of PCS can include chronic pelvic pain, discomfort during sexual intercourse, and heaviness or pressure in the pelvis.
On the other hand, chronic pelvic pain can also cause varicose veins. When women experience pelvic pain, they may avoid physical activity, leading to poor circulation in the legs and an increased risk of developing varicose veins. Therefore, there is a strong connection between varicose veins and pelvic pain in women, and it is important to seek medical attention if you are experiencing symptoms of either condition.
Treatment for Varicose Veins
Embolization is a minimally invasive procedure that is commonly used by interventional radiologists to treat varicose veins and pelvic pain caused by pelvic congestion syndrome (PCS). During the procedure, an interventional radiologist will insert a thin tube, called a catheter, into the affected vein through a small incision in the skin. Using X-ray or ultrasound guidance, the radiologist will guide the catheter to the damaged vein in the pelvis.
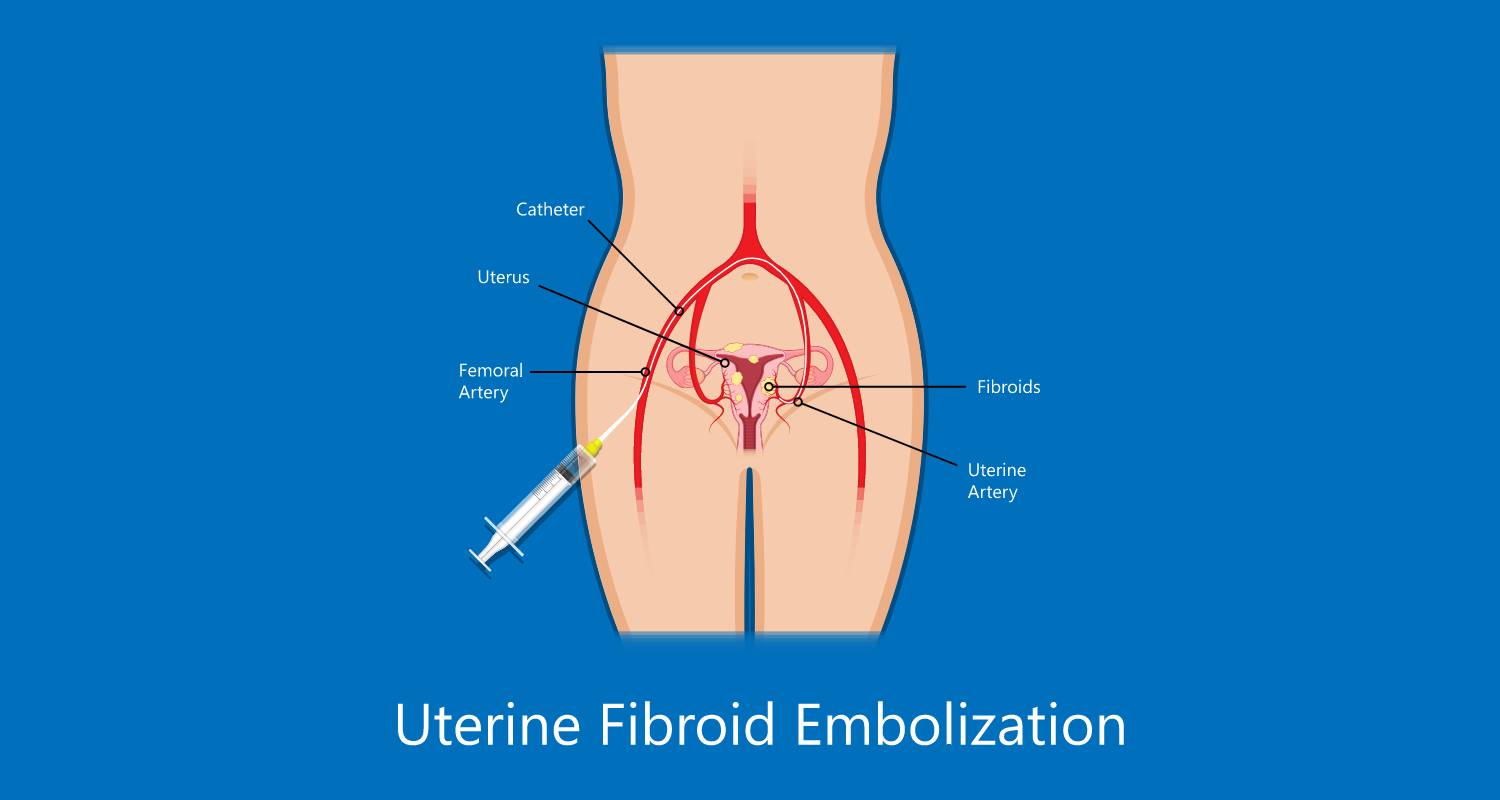
Once the catheter is in place, the interventional radiologist will use tiny coils or particles to block the vein and cut off the blood supply. This is done to reduce the pressure on the veins in the pelvis and relieve the symptoms of PCS, including chronic pelvic pain, discomfort during sexual intercourse, and a feeling of heaviness or pressure in the pelvis.
Embolization is a highly effective treatment for PCS, with success rates ranging from 85% to 95%. It is a minimally invasive procedure that can be performed on an outpatient basis, meaning patients can typically go home the same day. The procedure usually takes between 30 minutes and 2 hours to complete, depending on the extent of the damage to the vein.
In addition to treating PCS, embolization can also be used to treat varicose veins in other parts of the body, such as the legs. By blocking off the damaged vein, the procedure helps to redirect blood flow to healthy veins, reducing the appearance of varicose veins and relieving any associated discomfort or pain.
Overall, embolization is a safe and effective treatment option for varicose veins and pelvic pain caused by PCS. It is a minimally invasive procedure that can provide significant relief from symptoms and improve overall quality of life for patients.
In Conclusion
In conclusion, varicose veins and pelvic pain are strongly connected, with varicose veins in the pelvis being a common cause of chronic pelvic pain in women. Pelvic congestion syndrome, a condition in which the veins in the pelvis become enlarged and swollen, is a known cause of pelvic pain and discomfort, and it can be effectively treated by interventional radiologists using minimally invasive procedures such as embolization. It is also important to note that chronic pelvic pain can cause varicose veins by reducing physical activity, which can lead to poor circulation in the legs. Therefore, if you are experiencing symptoms of either condition, it is important to seek medical attention and explore treatment options that can alleviate your symptoms and improve your overall quality of life.












