What are fibroids?
-
- Studies demonstrate the prevalence of fibroids in 20-40% of women older than 35 years of age.1
- Evidence suggests that African-American women are three times more likely to develop uterine fibroids2-4 than other women, with an earlier age of onset.5
- Most clinicians believe fibroids shrink when a woman goes through menopause.
Symptoms
Common symptoms associated with uterine fibroids.
- Excessive Menstrual Bleeding
Heavy menstrual bleeding is one of the most common symptoms associated with uterine fibroid tumors. It is the most prevalent symptom for two of the four types of uterine fibroid tumors: intramural and submucosal. Over time, excessive menstrual bleeding can lead to fatigue and anemia, which is a result of low red blood cell count. If left untreated, excessive menstrual bleeding can eventually lead to the need for blood transfusions.
- Pelvic Pain and Pressure
As fibroids grow, they can put additional pressure on the surrounding organs, which can be extremely painful. The growth of the fibroids can cause consistent lower abdominal pain, as well as swelling which is sometimes mistaken for as weight gain or pregnancy. If you are experiencing pelvic pain or pressure or any other type of uterine fibroid symptoms, a full gynecological exam should be done immediately to determine the cause.
- Urinary Incontinence or Frequent Urination
One of the organs commonly affected during the growth of fibroid tumors is the bladder. As added pressure is applied to this organ, the risk of urinary incontinence (loss of bladder control) occurs, as well as frequent urination.
- Other Symptoms
Other common symptoms include anemia, pain in the back of the legs, pain during sexual intercourse, constipation, and an enlarged abdomen.
If you are experiencing signs and symptoms of uterine fibroids, and are finding it difficult to perform your daily activities and maintain your way of life, we recommend you contact 1Fibroid Center as soon as possible and we will help you find the best treatment option.
Types of Fibroids
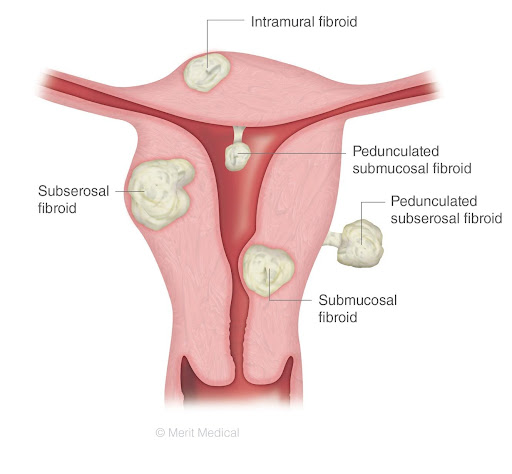
There are four primary types of fibroids.
- Intramural
The most common type of fibroids, intramural fibroid tumors, typically develop within the uterine wall and expand from there. When an intramural fibroid tumor expands, it tends to make the uterus feel larger than normal, which can sometimes be mistaken for pregnancy or weight gain. This type of fibroid tumor can also cause “bulk symptoms” which include excessive menstrual bleeding that may cause prolonged menstrual cycles and clot passing, and pelvic pain that is caused by the additional pressure placed on surrounding organs by the growth of the fibroid.
- Subserosal
Subserosal fibroids typically develop on the outer uterine wall. This type of fibroid tumor can continue to grow outward and increase in size. The growth of a subserosal fibroid tumor will put additional pressure on the surrounding organs, causing pelvic pain and pressure, and tend not to interfere with a women’s typical menstrual flow. Depending on the severity of the location of the fibroids, other complications may accompany pain and pressure such as bloating, indigestion, constipation, and frequent urination.
- Submucosal
These fibroids develop under the lining of the uterine cavity. Large submucosal fibroid tumors may increase the size of the uterus cavity and can block the fallopian tubes, which can cause complications with fertility. Associated symptoms with submucosal fibroids include very heavy, excessive menstrual bleeding and prolonged menstruation. These symptoms can also cause the passing of clots and frequent soiling accidents. Untreated, prolonged or excessive bleeding can cause more complicated problems such as anemia and/or fatigue, which could potentially lead to a future need for blood transfusions.
- Pedunculated
This type of uterine fibroid occurs when a fibroid tumor grows on a stalk, resulting in pedunculated submucosal or subserosal fibroids. These fibroids can grow into the uterus and/or outside of the uterine wall. Symptoms associated with pedunculated fibroid tumors include pain and pressure as the fibroid may sometimes twist on the stalk.
A woman may have one or all of these types of fibroids. Some fibroid tumors don’t produce any symptoms at all, while others can be severely symptomatic. It is common for a woman to have multiple fibroid tumors and it may be difficult to understand which fibroid is causing specific symptoms.
Don’t suffer in silence with fibroids. Instead, reclaim your life! Learn as much as you can about uterine fibroids and treatment options, work together with your family and healthcare team to make the best of your care, and take control of your life.
References:
- Wallach EE. Myomectomy. In: Thompson JD, Rock JA, eds. Te Linde’s Operative Gynecology, 7th ed. Philadelphia: J.B. Lippincott, 1992; pp 647-662.
- Baird DD, Dunson DB, Hill MC, Cousins D, Schectman JM. High cumulative incidence of uterine leiomyoma in black and white women: Ultrasound evidence. Am J Obstet Gynecol. 2003;188:100–107.
- Marshall LM, Spiegelman D, Barbieri RL, et al. Variation in the incidence of uterine leiomyoma among premenopausal women by age and race. Obstet Gynecol. 1997;90:967–973.
- Wise LA, Palmer JR, Stewart EA, Rosenberg L. Age-specific incidence rates for self-reported uterine leiomyomata in the Black Women’s Health Study. Obstet Gynecol. 2005;105: 563–568.
- Huyck KL, Panhuysen CI, Cuenco KT, et al. The impact of race as a risk factor for symptom severity and age at diagnosis of uterine leiomyomata among affected sisters. Am J Obstet Gynecol. 2008;198:168 e161–169.
© Merit Medical, Used With Permission.











